In 2021, 38.4 million people (11.6% of the U.S. population) had diabetes, but its impact is especially severe in American Indian and Alaska Native (AI/AN) communities. While about 1 in 10 Americans has diagnosed diabetes overall, AI/AN adults face nearly three times the risk of type 2 diabetes compared to White adults.
This disparity makes AI/AN specific diabetes education, prevention, and care critical. Culturally grounded health strategies can help close this gap and improve quality of life for Indigenous communities.
Table of Contents
What Is Diabetes?
Diabetes is a chronic metabolic disease in which the body’s ability to produce or respond to insulin is impaired, leading to elevated blood glucose (blood sugar) in the bloodstream. Glucose is the body’s main source of energy, derived both from food and natural production. Insulin, a hormone produced by the pancreas, helps move glucose from the bloodstream into cells, where it is used for energy or stored for later use.
When the body does not produce enough insulin, or cannot use it properly, glucose builds up in the blood instead of being absorbed by the cells. This leads to the condition known as diabetes.
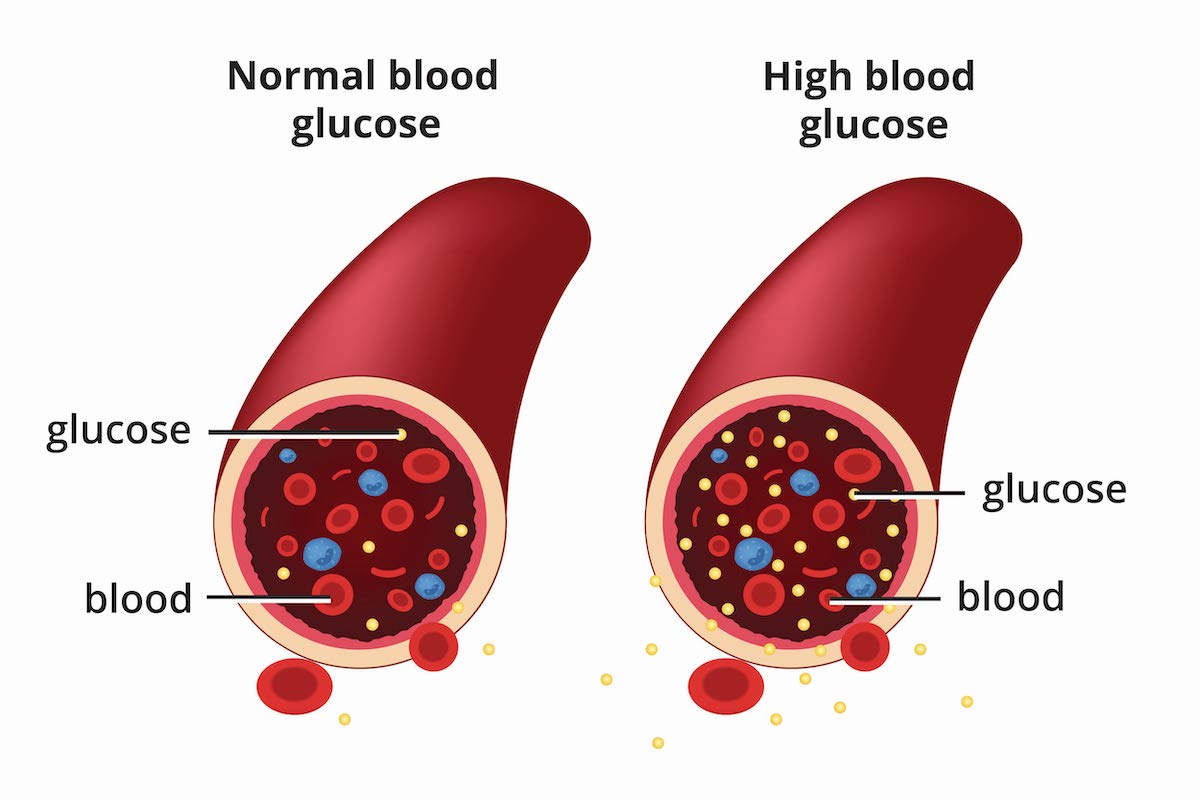
There are two main types:
- Type 1 diabetes: An autoimmune condition in which the body’s immune system mistakenly destroys the insulin producing cells in the pancreas.
- Type 2 diabetes: The most common type of diabetes, especially in adults, and occurs when the body becomes resistant to insulin and eventually produces less of it. Risk factors include obesity and a family history of the disease.
Over time, uncontrolled diabetes can lead to serious complications such as heart disease, kidney failure, vision loss, nerve damage, and even increase risk for certain cancers.
According to the Office of Minority Health, AI/AN adults were diagnosed with diabetes 36% more often than the total U.S. population in 2024.
Understanding Diabetes in Native American Populations: Why is Diabetes So Common?
Diabetes among Native American populations is at an epidemic level. While many factors contribute to these high rates, the roots of this crisis lie in a combination of historical trauma, lifestyle shifts, genetic predispositions, and systemic healthcare challenges.
Historical and socioeconomic forces
For many Native populations, the transition from traditional ways of life to reservation life introduced major disruptions to food systems, physical activity, and overall health. Where once diets were rich in natural foods and daily life included high levels of physical activity, post reservation diets forced a shift toward processed foods high in refined white flour, sugar, and fat. Other contributing factors to the rising rates of diabetes include poverty, geographic isolation, and lack of access to fresh foods.
Lifestyle changes and food sovereignty
The loss of access to land and traditional food systems also plays a major role. Native communities no longer had the resources or space to cultivate or harvest traditional foods. Processed, inexpensive foods have become the default option, contributing to obesity and sedentary lifestyles.
Genetic and metabolic predisposition
According to the National Library of Medicine, AI/AN adults have a higher likelihood of developing metabolic syndrome, which increases the risk of diabetes, heart disease, and stroke.
Limited healthcare access
Many Native Americans, particularly those living on rural reservations, experience significant arrears to healthcare including limited access to preventive services, delayed diagnoses, and a lack of competent care. Read more about Native American healthcare access here.
Native American Diabetes Rates
The statistics reveal just how diabetes in Native American populations affects AI/AN communities:
- AI/AN adults have the highest diagnosed diabetes rates of any U.S. racial group/ The prevalence for both men and women is 13.6%.
- The diabetes-related mortality rate among AI/AN adults is 3.2 times greater than the U.S. all races average.
- Among adults living on tribal lands, the diabetes diagnosis rate is 18.9%, significantly higher than the 11.5% rate among Native people living off tribal lands.
- Some tribes, particularly in the Southwest, report much higher rates of diabetes. According to the National Indian Council on Aging, one tribe has a rate of over 50% of its members diagnosed with type 2 diabetes, the highest in the world.
The Impact on AI/AN Communities
The impact of diabetes goes far beyond initial diagnosis in Native populations, it’s one of the leading causes of severe complications like kidney failure, heart disease, and premature death. AI/AN communities experience some of the highest rates of end-stage renal disease (ESRD), primarily driven by type 2 diabetes. According to the National Library of Medicine, the prevalence of ESRD in AI/AN populations is 3.5 times higher than in white Americans.
A 2023 survey by Podimetrics, revealed that 42% of AI/AN patients with type 2 diabetes had visited the emergency room due to complications, and among them, two-thirds had gone three or more times which highlights the frequency and severity of acute complications in these populations.
Further data from the 2024 Indian Health Service (IHS) Assessment of Diabetes Complications Audit emphasizes this widespread burden:
AI/AN individuals tend to be diagnosed with diabetes at younger ages and suffer more severe complications than other populations. This early onset and high complication rate deepen the long term burden on families, tribal healthcare, and communities.
The Role of Culture and Community in Diabetes Prevention
Diabetes prevention efforts in Native communities are most successful when they are rooted in culture and community values. In recognition of this and the epidemic of type 2 diabetes in Native populations, Congress established the Special Diabetes Program for Indians in 1997. Administered by the IHS Division of Diabetes Treatment and Prevention (DDTP), this program has expanded access to quality care and culturally informed prevention services across hundreds of IHS, Tribal, and Urban Indian health programs nationwide.
The DDTP helps implement evidence-based practices and community level initiatives that blend public health, clinical treatment, and traditional healing. This framework ensures that diabetes prevention strategies are both effective and aligned with Indigenous values.
From 2008 to 2014, the CDC’s Native Diabetes Wellness Program Traditional Foods Project partnered with 17 tribes and tribal organizations to support the restoration of Indigenous foodways as a strategy to prevent type 2 diabetes. Through this initiative communities were encouraged to reclaim nutrient dense traditional foods such as corn, beans, and wild rice. These efforts went far beyond improving nutrition. They became a way to restore cultural identity, strengthen community, and promote tribal food sovereignty. By reconnecting food to land, and lifeways, tribal partners demonstrated how traditional foods can be powerful tools for both health education and diabetes prevention.
Preventions & Solutions
At Native Reach™, we believe Indigenous health education is not optional, it’s essential. We partner with Indigenous voices and organizations to deliver culturally reflective media and campaigns that speak to Indigenous values and voices. Through platforms like GoodhealthTV®, online learning, and custom mobiles apps, we help amplify Native perspectives and make health messages stick. Contact us to explore how our tools can support your outreach goals.

A key nationwide initiative is the National Diabetes Prevention Program (DPP), CDC led effort to reduce type 2 diabetes through lifestyle change programs. The National DPP is tailored for tribal communities through adaptations that incorporate Native values and storytelling.
3 Solutions and Strategies for the Future
1. Empower Native Educators and Health Workers
By investing in the training and support of Native educators, lifestyle coaches, and community health representatives, communities can deliver better care and education. These roles are essential for preventing diabetes in Native populations, early interventions, and long-term disease management.
3. Advocate for Policy and Funding Support
Sustained investment is critical for continuing the progress made by programs like the SDPI. Policy solutions should prioritize expansion of IHS resources and infrastructure as well as broader access to care across all levels of the healthcare system.
2. Using Technology for Better Outcomes
Technology offers powerful tools to overcome healthcare access barriers in rural tribal communities. According to the Podimetrics survey, AI/AN patients favored the following tech-based strategies to improve diabetes care:
- 48% preferred remote patient monitoring devices to track their health at home
- 36% supported expanded telehealth access
- 35% wanted more frequent touchpoints between clinical visits
These preferences show the value of integrating digital health tools with culturally competent care delivery.
Changing the Narrative on Native Diabetes
Diabetes in Native populations poses a critical health challenge, but it is not unchangeable. With culturally centered education, empowered local leadership, and systemic support, AI/AN populations can shift toward wellness and prevention.
Contact Native Reach to explore partnerships on culturally aligned health education campaigns and multimedia outreach that resonate with Native audiences. Let’s work towards healthier futures together.
